Menu
Nathan Radcliffe, MD, is a glaucoma specialist at New York Eye Surgery Center with busy practices in the Bronx and Queens. Over the course of his career, visual field testing has remained a core component of glaucoma evaluation and management. During fellowship training, Dr. Radcliffe learned the language of perimetry. Progression can be measured as a trend or as an event, assessed at individual points or globally across the visual field.
Reliable visual field data is essential for these analyses. Detecting progression often requires multiple reliable tests over several years. The original vision for perimetric software was that physicians could follow patients longitudinally and rely on automated progression analysis to help guide treatment escalation or surgical decisions.
In reality, clinical practice often introduces challenges that make this ideal workflow difficult to achieve. High patient volume, inconsistent testing reliability, and logistical limitations can complicate the collection of consistent data needed for long-term progression analysis.

In a busy glaucoma practice, maintaining consistent visual field testing is not always straightforward.
Traditional bowl-based perimetry can be uncomfortable for some patients, particularly elderly individuals or those with musculoskeletal limitations. The test can also be time-consuming, leading to patient hesitation or refusal. In Dr. Radcliffe’s experience, patient refusal to perform the traditional visual field test is not uncommon.
Reliability and repeatability also remain longstanding challenges in perimetry. Even in controlled studies, variability between tests can make it difficult to determine whether a change represents true progression or simply measurement fluctuation.
In addition, real-world glaucoma management introduces variables that can complicate the interpretation of visual field progression. Treatment changes, medication noncompliance, and improvements in intraocular pressure can all affect visual field outcomes during the same period that physicians are attempting to measure progression.
Operational challenges can further complicate testing frequency. Technician shortages, workflow constraints, and high patient volumes can make it difficult to perform visual field testing at the ideal intervals needed for detailed progression analysis.
Despite these challenges, visual field testing remains a critical component of glaucoma care. For new glaucoma evaluations, a visual field defect can confirm a structure-function relationship and help guide treatment decisions. For patients with established disease, the visual field remains one important data point alongside intraocular pressure, imaging, clinical examination, and treatment history.
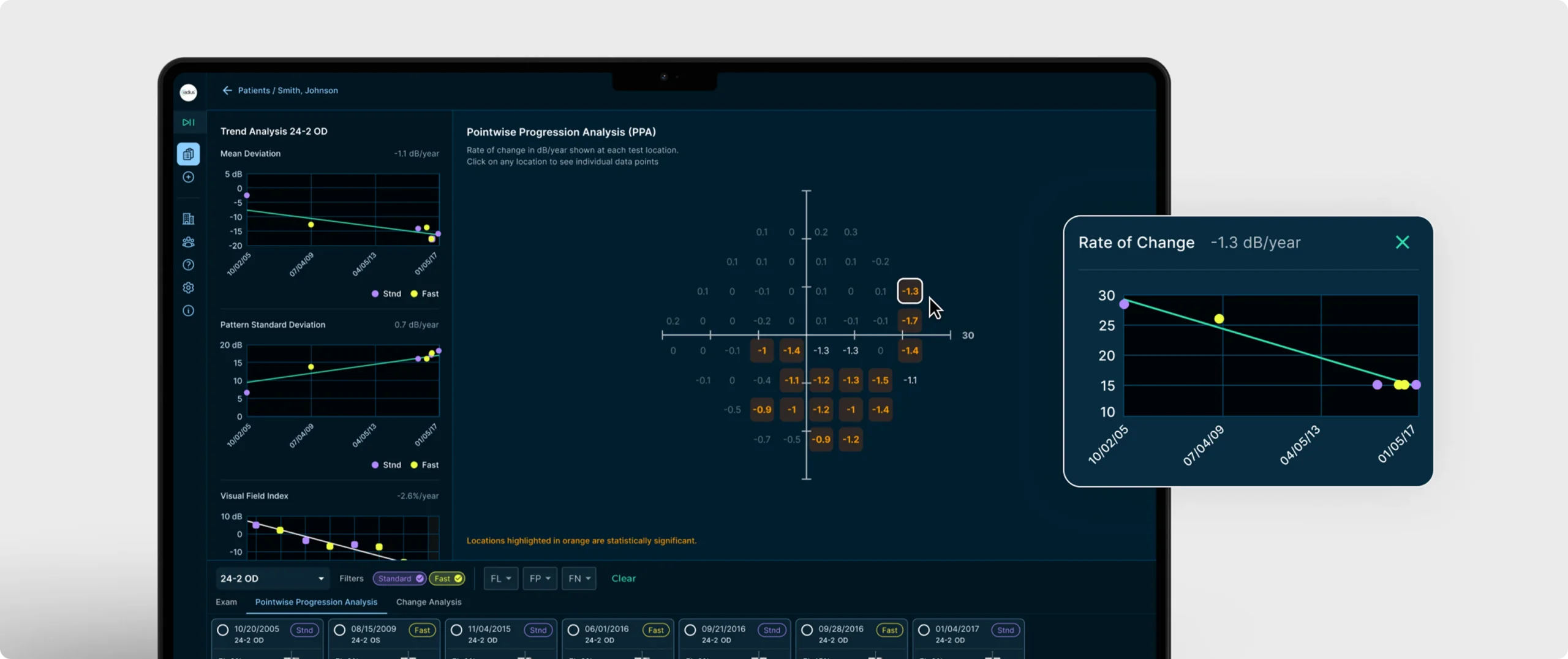

Several years ago, these practical challenges prompted Dr. Radcliffe to explore newer approaches to perimetry, including headset-based virtual visual field testing.
After evaluating several platforms, his practices trialed and ultimately adopted the RadiusXR virtual perimetry system. Rather than replacing traditional bowl perimeters entirely, the Radius system was introduced alongside existing equipment.
Initially, Dr. Radcliffe ordered the virtual visual field test for all new glaucoma patients and for glaucoma suspects during follow-up visits. Starting these patients on a virtual baseline avoided disruptions in continuity that might occur when switching testing platforms mid-evaluation.
This approach worked well in practice. Patients generally preferred the new testing format, which is ergonomically friendlier and easier to tolerate for many individuals. Because the virtual test can often be completed in less time, overall clinic flow improved.
Integration Into Daily Practice
As the practice gained more experience with the system, virtual perimetry use expanded. Today, most new and follow-up glaucoma patients may receive a virtual visual field test, while traditional bowl perimetry is reserved for the smaller number of cases where maintaining continuity with prior testing is particularly valuable.
Dr. Radcliffe also noted that variability in test reliability is not unique to any single perimetry method. Both traditional and virtual visual field assessments can encounter challenges related to repeatability, patient attention, and testing conditions.
What became clear over time was that the RadiusXR system could support the same clinical role that visual field testing has always played in glaucoma care while improving workflow efficiency and patient experience.
Improved Testing Compliance
Introducing virtual perimetry increased patient willingness to complete visual field testing. The ergonomically friendly headset design helped reduce discomfort associated with traditional bowl testing, making it easier for patients to participate in recommended evaluations.
This improvement in patient acceptance helped practices maintain better adherence to visual field testing schedules.
Increased Clinical Efficiency
Because the virtual test can often be completed in less time and does not require the same dedicated testing setup as traditional perimetry, overall clinic throughput improved. Reduced testing time and improved workflow helped decrease wait times in the office.
For a high-volume glaucoma practice, these operational improvements made it easier to keep up with the demand for perimetry.
Reliable Data for Clinical Decision Making
For Dr. Radcliffe, the most important outcome is the ability to continue using visual field data as part of a broader clinical evaluation.
As he explains:
“As a direct user of RadiusXR, I can attest to its efficiency and reliability for diagnosing and monitoring visual field defects in patients with glaucoma.”
Visual field testing remains one component of a comprehensive glaucoma assessment that also includes intraocular pressure measurements, imaging findings, treatment adherence, and clinical examination.
A Practical Addition to Modern Perimetry
Today, both traditional and virtual perimetry coexist within Dr. Radcliffe’s practices. The flexibility to use either modality allows the clinic to maintain continuity where needed while improving efficiency and patient comfort.
Adopting the RadiusXR system ultimately proved less disruptive than initially expected. According to Dr. Radcliffe, the transition allowed his practices better to meet the needs of both patients and staff while continuing to incorporate visual field testing as a meaningful component of glaucoma care.
Mon – Fri 5:00 am – 5:00 pm PST